
Note: I’m writing a series on my bout with ovarian cancer and how my running was affected by it and helped me deal with it. You can read Part 1 for a little history on my running and cancer here.
I’ve focused on running throughout my whole cancer journey. Okay, I obsessed over it. When I went for my 2 week follow-up with the surgeon, I asked him first about when I could run again and left out all the other questions about work and driving! Oops! Same thing with my initial visit with my oncologist – I wanted to know if and when I could run.
Why was it my priority? What made it so important for me? Mostly for the reasons I stated in the Part 1 post but also because it gave me a sense of control…over something, anything instead of feeling controlled by cancer. It gave me something to focus on when I was terrified they would find cancer and what stage it would be. It gave me something to focus on while I was recuperating from surgery. And it gave me something to focus on when I learned I would have chemotherapy. I felt like my life was out of control and running gave me something I COULD have control over.
So now I could run again but what could I do? What should I do? I had told my oncologist about signing up for the Tinkerbell Half Marathon (which would happen after my fourth round of chemo). She didn’t shoot that idea down and in fact, she thought it was a great one. She said she loved when her patients were marathoners and half marathoners. Okay, great!
But…neither my oncologist nor my surgeon gave me specifics on what I could or should do. What I’m comfortable with was just too vague. But I couldn’t really find out a whole lot except that exercise was encouraged for cancer patients because it helped combat the fatigue and tiredness from chemotherapy. Could I do TOO much? Should I be cautious? Should I run as fast as I could or slow as molasses? What is an excited runner girl supposed to do?
I started looking around and I didn’t find a whole lot. There was this from the American Cancer Society’s Answers To Common Questions section:
“Research strongly suggests that exercise is not only safe during cancer treatment, but it can also improve physical functioning and many aspects of quality of life. Moderate exercise has been shown to improve fatigue (extreme tiredness), anxiety, and self-esteem. It also helps heart and blood vessel fitness, muscle strength, and body composition (how much of your body is made up of fat, bone, or muscle).”
So I knew that I should do something but what does moderate mean? Is running slow moderate? Could I run tempo runs? Could I lift weights? I found more information on their Guidelines page:
Be physically active
• Adults should get at least 150 minutes of moderate intensity or 75 minutes of vigorous intensity activity each week (or a combination of these), preferably spread throughout the week.
• Children and teens should get at least 1 hour of moderate or vigorous intensity activity each day, with vigorous activity on at least 3 days each week.
• Limit sedentary behavior such as sitting, lying down, watching TV, and other forms of screen-based entertainment.
• Doing some physical activity above usual activities, no matter what one’s level of activity, can have many health benefits.
Okay, more information is good. But still…what is moderate? What is vigorous? They also had this chart to help figure that out:
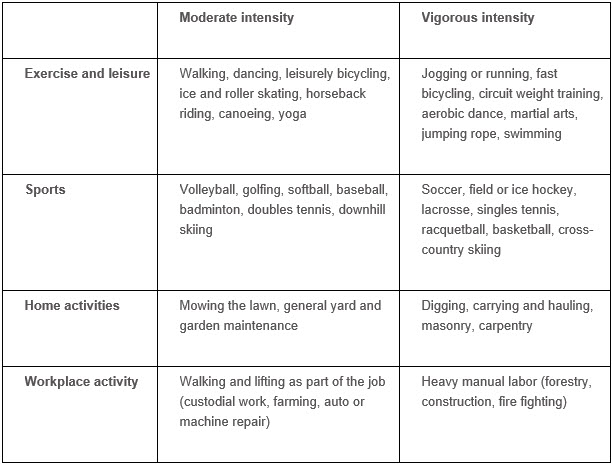
According to this chart, running is vigorous. Hmmm…
Running slow and easy doesn’t seem vigorous to me. I decided to consider it moderate and see how I did. I found another article from the American College of Sports Medicine – Exercise During Cancer Treatment that gave more specifics about what to watch out for:
Individuals undergoing cancer treatment should:
•Obtain approval from their oncologist (cancer doctor) before starting an exercise program.
•Have vital signs (temperature, pulse/heart rate, blood pressure, respiration rate) monitored regularly. If participating in moderate-to-vigorous exercise, have their blood pressure and heart rate monitored before, during and after exercise to ensure that participation in exercise is appropriate and safe.
•Exercise with a partner, caregiver or exercise professional for safety reasons.
•Avoid public fitness facilities and activities (e.g., swimming), where there may be an increased risk of exposure to viral and/or bacterial infection.
•Avoid swimming if undergoing radiation therapy treatments or if they have an indwelling catheter (a tube that goes in the body), such as a central venous catheter or peripherally inserted central catheter.
•Stop exercise and contact their doctor if they have any of the following symptoms during exercise or after an exercise session:
– Disorientation, dizziness, blurred vision or fainting
– Sudden onset of nausea, vomiting
– Unusual or sudden shortness of breath
– Irregular heart beat, palpitations, chest pain
– Leg/calf pain, bone pain, unusual joint pain or pain not caused by injury
– Muscle cramps or sudden onset of muscular weakness or fatigue
And also from that page, this section on when to take precautions:
•Anemia (low red blood cell count): If the red blood cell count is low, the body’s ability to carry oxygen to the tissues is reduced. Exercise may need to be scaled back and possibly avoided.
•Neutropenia (low white blood cell count): If the white blood cell count is low, the body’s ability to fight infection is reduced. Exercise should be avoided if there is a fever above 100.4°F (>38°C).
•Thrombocytopenia (low platelet count): If platelet count is low, there is an increased risk of bruising and bleeding. Avoid contact sports or activities with high risk of injury or falling. Report any unusual bruising or symptoms, such as nose bleeds, to a doctor.
•Side effects such as vomiting and diarrhea, and symptoms such as swollen ankles, unexplained weight loss/gain, or shortness of breath with low levels of exertion may make exercise unsafe. Check with a doctor before exercising.
Ok, great. I could all that. I now felt like I had enough to go on. I decided that 2 5K runs during the weekday would be good and I’d let myself do a longer trail run on the weekends. While the combination might be more time than I’d been allotted per the guidelines, I hoped the combination of “moderate” 5K runs and more vigorous trail runs would be okay. I would just listen to my body day to day and do what I felt I could. But I have to tell you, I sometimes wanted to do more!
This was the plan through mid-January and it went pretty well. I wasn’t pushing myself too much and really just having fun. I was tired but not overly so, though I sometimes felt the same kind of tired after a 5K run that I used to feel after a 20 miler which was frustrating. I ran when I could and rested when I felt I needed it. Mostly, the pattern went like this:
- The day after chemo I could run and feel tired but okay.
- Then chemo would hit me and I would take the next 4 or 5 days off from.
- Then on the 6th or 7th day after chemo, I would feel I could run again.
- Then I would resume the schedule I set above.
But in mid-January, I got the racing bug and started thinking about my plans for 2014. What if I did more? What if I added pilates or yoga or weight training? What if I ran a little faster sometimes? What if…
***
Click Here to read Running with Cancer – PART 3: One Day at a Time
And don’t forget, if you missed Part 1, you can read it here:
If you’ve been through cancer and chemotherapy and are a runner, I would love to hear how it went for you. Please let me know in the comments or email me at the link below.

























